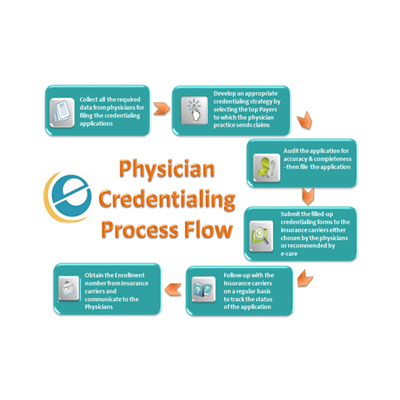
Provider enrollment and credentialing is a critical process in the healthcare industry that ensures medical professionals are verified, approved, and authorized to work with insurance companies and healthcare networks.
Credentialing focuses on verifying a provider’s qualifications—such as education, licenses, certifications, and work history. On the other hand, enrollment is the process of registering that provider with insurance payers so they can legally bill and receive payments for services.
Without proper provider enrollment & credentialing, healthcare providers cannot get reimbursed, which directly impacts revenue flow.
Why Provider Enrollment and Credentialing Matters
This process is not just a formality—it directly affects your practice’s credibility, compliance, and income.
- Ensures providers meet industry standards
- Builds trust with patients and insurance companies
- Prevents claim rejections and delays
- Maintains compliance with healthcare regulations
- Enables smooth revenue cycle management
Even a small error in credentialing and enrollment can lead to payment delays or denials, costing your practice both time and money.
Key Steps in the Credentialing and Enrollment Process
1. Provider Credentialing
This step involves collecting and verifying:
- Medical licenses
- Board certifications
- Education and training history
- Work experience
- Malpractice insurance
Primary source verification is done to ensure accuracy and compliance.
2. Provider Enrollment
After credentialing, providers are enrolled with insurance payers such as Medicare, Medicaid, and private insurance companies.
This includes:
- Submitting applications
- Completing payer-specific forms
- Attaching verified documents
- Following up with payers
3. Approval and Contracting
Once approved:
- Providers receive network participation status
- Contracts are finalized with payers
- Billing can officially begin
Common Challenges in Provider Enrollment & Credentialing
Many healthcare practices struggle with this process due to:
- Complex paperwork and documentation
- Frequent policy changes by insurance companies
- Long processing times (sometimes 60–120 days)
- Application errors leading to rejections
- Lack of follow-ups
This is why many clinics prefer outsourcing enrollment and credentialing services to professionals.
Benefits of Professional Credentialing and Enrollment Services
Working with experts like BillCare can simplify the entire process and help avoid costly mistakes.
Here’s what you gain:
- Faster enrollment approvals
- Reduced claim denials
- Accurate documentation handling
- Continuous follow-ups with payers
- Compliance with industry regulations
With reliable credentialing and enrollment services, your team can focus more on patient care instead of administrative work.
Who Needs Provider Enrollment and Credentialing?
This process is essential for:
- Doctors and physicians
- Clinics and medical practices
- Hospitals and healthcare facilities
- Mental health professionals
- Telehealth providers
If you plan to accept insurance payments, enrollment and credentialing is mandatory.
Why Choose BillCare for Provider Enrollment and Credentialing Services
At BillCare, we specialize in managing the complete enrollment and credentialing process with precision and efficiency.
Our approach focuses on:
- Error-free submissions
- Faster approvals
- Dedicated support
- Transparent communication
We ensure your practice stays compliant while maximizing revenue potential through seamless provider enrollment & credentialing.
Final Thoughts
Understanding provider enrollment and credentialing is essential for running a successful healthcare practice. It’s not just about paperwork—it’s about ensuring your services are recognized, approved, and reimbursed without delays.
By investing in expert enrollment and credentialing services, you reduce administrative burden, improve cash flow, and maintain a strong professional reputation.
Get Started with Expert Provider Enrollment and Credentialing Services
Managing provider enrollment and credentialing on your own can be time-consuming and complex. At BillCare, we simplify the entire process with accuracy and speed.
Whether you’re starting a new practice or expanding your network, our enrollment and credentialing services ensure you get approved faster and start billing without delays.
👉 Let our experts handle your credentialing and enrollment while you focus on patient care.