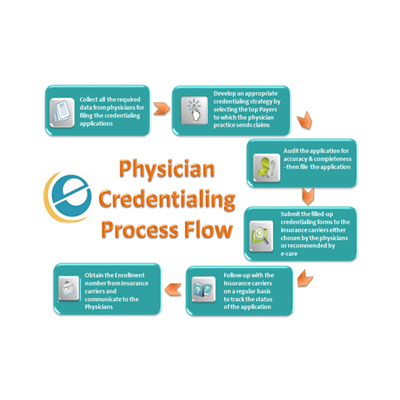
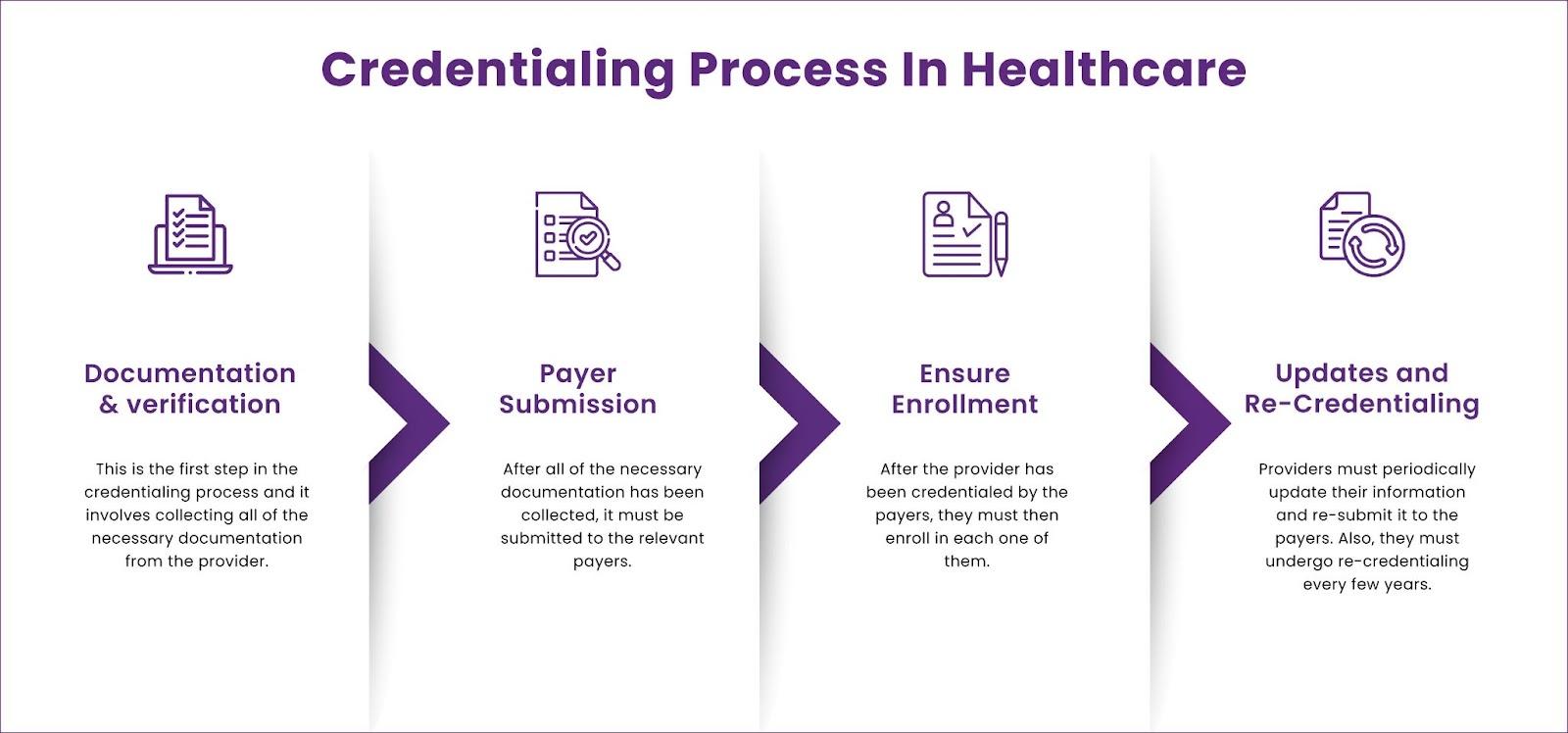
Healthcare providers in Illinois face strict regulatory requirements and increasing payer complexity. Delays in enrollment or credentialing can directly impact revenue, patient trust, and operational efficiency.
billcare delivers reliable provider enrollment and credentialing services designed to eliminate bottlenecks, reduce claim denials, and accelerate approvals across both government and commercial payers
Streamline Your Provider Enrollment Journey
Managing enrollment manually leads to errors, missed deadlines, and revenue loss. A structured approach ensures faster approvals and compliance with payer requirements like Centers for Medicare & Medicaid Services.
With billcare, healthcare organizations gain:
- Faster onboarding with major payers
- Reduced administrative burden
- Improved claim acceptance rates
- Full compliance with evolving regulations
Our provider enrollment and credentialing services are built to support clinics, hospitals, and private practices across Illinois.
Best Provider Enrollment Journey
The best enrollment journey is not just fast. It is accurate, compliant, and scalable.
billcare focuses on:
- End-to-end tracking of applications
- Real-time status updates
- Error-free documentation submission
- Faster payer approvals
This ensures your providers start seeing patients and generating revenue without unnecessary delays.
Seamless Provider Enrollment & Credentialing with billcare
billcare integrates advanced workflows with deep industry expertise to deliver seamless credentialing support.
We handle:
- Initial enrollment and revalidation
- Credential verification and documentation
- Payer communication and follow-ups
Our system aligns with standards from organizations like National Committee for Quality Assurance, ensuring high-quality credentialing outcomes.
Our Comprehensive Suite of Provider Enrollment and Credentialing Services
billcare offers a complete ecosystem of provider enrollment and credentialing services tailored for US healthcare providers, especially those operating in Illinois.
Government Program Participation
We manage enrollment with federal and state programs, including:
- Medicare
- Medicaid
Our team ensures timely submissions, accurate documentation, and ongoing compliance.
Commercial Insurance Integration
Credentialing with private payers can be complex. We simplify:
- Contracting with major insurance companies
- Network participation approvals
- Payer-specific requirements handling
This reduces delays and increases patient coverage access.
Core Registrations & Profiles
We handle essential provider registrations such as:
- National Provider Identifier
- CAQH profile setup and maintenance
Accurate profiles ensure smooth payer processing.
Licensing & Certification Management
Maintaining valid licenses is critical. We assist with:
- State license applications and renewals
- Board certifications
- Compliance tracking
This minimizes risk and keeps your practice operational.
Hospital Affiliation Support
Hospital privileges require proper documentation and approvals. billcare ensures:
- Accurate application submissions
- Credential verification
- Continuous follow-up with hospitals
Ongoing Credentialing & Compliance
Credentialing is not a one-time task. We provide:
- Recredentialing management
- Audit preparation
- Compliance monitoring
Our provider enrollment and credentialing services ensure your practice stays compliant and revenue-ready.
The billcare Advantage
Choosing billcare is a strategic decision, not just an operational one.
What sets us apart:
- Dedicated credentialing experts
- Faster turnaround times
- Reduced claim denials
- Scalable solutions for growing practices
- Deep understanding of Illinois healthcare regulations
We don’t just process applications. We optimize your entire enrollment lifecycle to maximize revenue and efficiency.
FAQ’s
1. How long does provider enrollment take in Illinois?
It typically takes 30 to 120 days depending on the payer. billcare helps reduce delays through accurate and timely submissions.
2. Why are credentialing services important?
Without proper credentialing, claims get denied and providers cannot legally bill insurers.
3. Do you handle both Medicare and private insurance enrollment?
Yes, billcare manages both government and commercial payer enrollments.
4. Can billcare manage recredentialing?
Yes. We provide ongoing support to ensure continuous compliance and avoid disruptions.
5. Who should use provider enrollment services?
Clinics, hospitals, group practices, and individual providers looking to reduce administrative burden and speed up approvals.