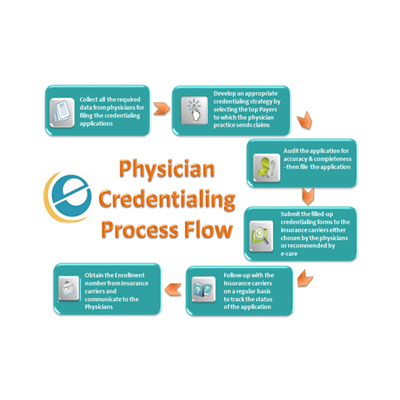
Physicians must complete a strict verification process before they can treat insured patients or submit claims to insurance companies. Physician credentialing services simplify this process by handling provider verification, insurance enrollment, and compliance management.
Credentialing confirms a physician’s professional qualifications including education, medical licenses, board certifications, and work experience. Insurance companies require this verification before allowing a physician to participate in their network.
Because credentialing involves detailed paperwork, payer communication, and compliance tracking, many healthcare providers rely on professional credentialing experts.
Organizations like BillCare medical billing and credentialing services help physicians complete credentialing efficiently so they can begin seeing patients and receiving reimbursements without unnecessary delays.
What Is Physician Credentialing?
Physician credentialing is the process of verifying a doctor’s qualifications before they can join an insurance network or work with healthcare facilities.
Credentialing ensures that physicians meet professional standards and regulatory requirements.
The verification process typically includes:
-
Medical education verification
-
State license validation
-
Board certification confirmation
-
Work history review
-
Malpractice insurance verification
Insurance companies review this information before approving a physician as an in-network provider.
Without proper credentialing, physicians cannot bill insurance companies for patient services.
Steps in the Physician Credentialing Process
The credentialing process involves several stages.
Provider Information Collection
Credentialing specialists gather information about the physician’s education, training, licenses, and professional background.
Primary Source Verification
Information is verified directly with issuing organizations such as medical boards and universities.
Insurance Enrollment
Credentialing experts submit applications to insurance companies for network participation.
Payer Review
Insurance companies review submitted documentation and verify the physician’s credentials.
Approval and Network Participation
Once approved, physicians become in-network providers and can start billing insurers.
This process may take 60–120 days depending on the insurance payer.
Common Credentialing Challenges for Physicians
Many physicians face difficulties managing credentialing internally.
Common challenges include:
-
Complex insurance applications
-
Delays in payer approvals
-
Missing documentation
-
Credential renewal deadlines
Professional medical credentialing services help prevent these issues by ensuring accurate documentation and timely application submission.
How BillCare Helps Physicians
Managing credentialing while running a busy medical practice can be overwhelming.
BillCare medical billing and credentialing services help physicians simplify the entire credentialing process by managing:
-
Provider enrollment with insurance companies
-
CAQH profile management
-
Documentation verification
-
Credential renewals and compliance monitoring
By outsourcing credentialing, physicians can focus on patient care while experts handle administrative tasks.
Why Physician Credentialing Matters
Credentialing plays a critical role in healthcare operations.
Benefits include:
-
Access to insurance networks
-
Increased patient volume
-
Faster insurance reimbursements
-
Compliance with healthcare regulations
Physicians who complete credentialing efficiently can expand their practice and improve revenue potential.
FAQ – Physician Credentialing
How long does physician credentialing take?
Physician credentialing usually takes between 60 and 120 days depending on insurance payer requirements.
What documents are required for physician credentialing?
Documents include medical licenses, board certifications, malpractice insurance, education verification, and work history.
Can physicians outsource credentialing?
Yes, many physicians rely on professional credentialing providers such as BillCare to manage the process efficiently.