Why Choosing the Right Medical Credentialing Companies Matters
If you’re a healthcare provider, you already know how frustrating the credentialing process can be. Delays, paperwork errors, and insurance rejections can slow down your revenue before you even start seeing patients.
That’s why selecting the right medical credentialing companies is not just a choice — it’s a critical business decision.
At BillCare, we’ve seen practices struggle for months due to poor credentialing. The right partner can speed up approvals, reduce administrative stress, and help you start billing faster.
What Are Medical Credentialing Services?
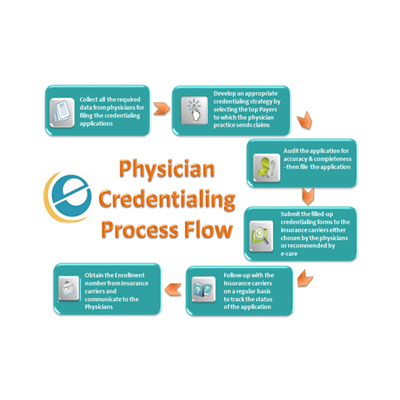
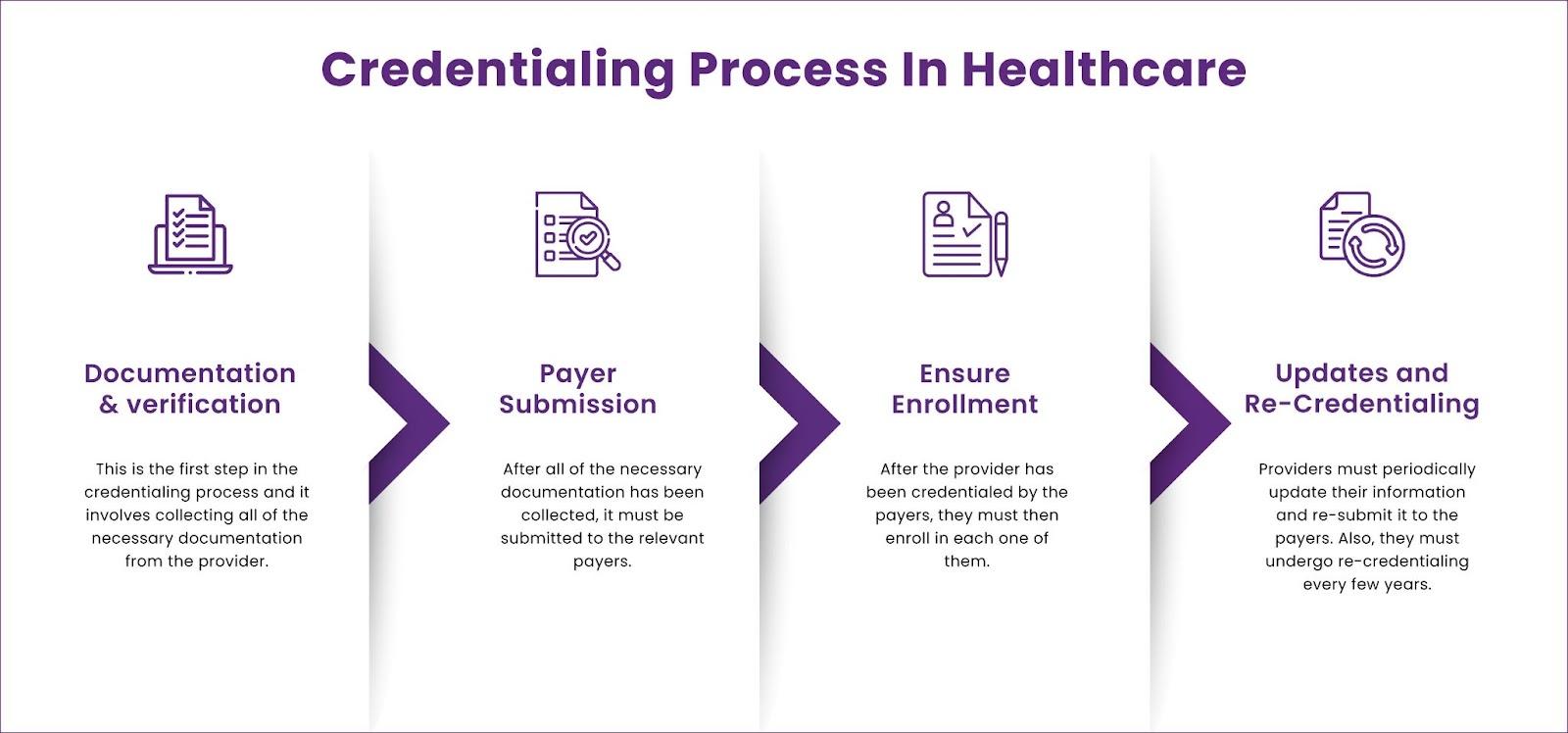
Medical credentialing services involve verifying a healthcare provider’s qualifications, experience, and compliance before they can work with insurance companies.
This process includes:
- License verification
- Education and training checks
- Insurance enrollment
- Background screening
Professional healthcare credentialing companies handle this entire process, ensuring accuracy and faster approvals.
Common Problems with Credentialing (Real-World Insight)
Many providers come to BillCare after facing issues like:
- Applications getting rejected due to minor errors
- Delays of 3–6 months in approvals
- Lack of communication from insurance panels
These problems directly impact revenue. Without proper medical billing and credentialing services, clinics often lose thousands in potential income.
How the Best Credentialing Services Make a Difference
Choosing the best credentialing services can transform your operations. Here’s how:
1. Faster Approvals
Experienced medical credentialing companies know exactly how to submit clean applications, reducing delays.
2. Error-Free Documentation
Every detail matters. A small mistake can delay approvals for weeks.
3. Continuous Follow-Ups
Top healthcare credentialing companies don’t just submit applications — they follow up until approval.
Why BillCare Stands Out
Not all medical credentialing companies deliver real results. At BillCare, we focus on performance, not just promises.
✔️ Proven Process
We use a structured workflow that ensures every application is complete and compliant.
✔️ Dedicated Support
Our team stays in touch throughout the process — no guesswork, no confusion.
✔️ Revenue-Focused Approach
We don’t just handle credentialing — we align it with medical billing credentialing services to ensure faster payments once approved.
Medical Billing and Credentialing Services: Why You Need Both
Many providers make the mistake of separating billing and credentialing.
But combining medical billing and credentialing services gives better results:
- Faster claim submissions after approval
- Reduced billing errors
- Improved cash flow
At BillCare, we integrate both processes to eliminate gaps and delays.
Signs You Need a Credentialing Partner
You should consider professional medical credentialing services if:
- Your applications keep getting delayed
- You’re unsure about insurance requirements
- Your staff is overwhelmed with paperwork
Reliable best credentialing services remove these burdens and let you focus on patient care.
How to Choose the Right Medical Credentialing Companies
Before hiring, evaluate these factors:
Experience
Look for healthcare credentialing companies with proven results.
Transparency
You should always know the status of your application.
Communication
Avoid companies that disappear after submission.
Integration with Billing
Choose providers offering medical billing credentialing services for better efficiency.
Real Impact: What You Can Expect
When you work with a reliable partner like BillCare, you can expect:
- Faster insurance approvals
- Reduced administrative workload
- Improved revenue cycle performance
This is why many providers are switching to professional medical credentialing companies instead of handling it in-house.
Final Thoughts
Credentialing is the foundation of your revenue cycle. Without proper setup, even the best billing system won’t perform.
Choosing the right medical credentialing companies ensures:
- Faster approvals
- Fewer errors
- Better financial outcomes
If you’re looking for a trusted partner, BillCare provides complete medical credentialing services and integrated billing solutions designed to help your practice grow.
Ready to Get Started?
If delays are holding back your practice, it’s time to act.
Let BillCare handle your credentialing and billing so you can focus on what matters most — your patients.