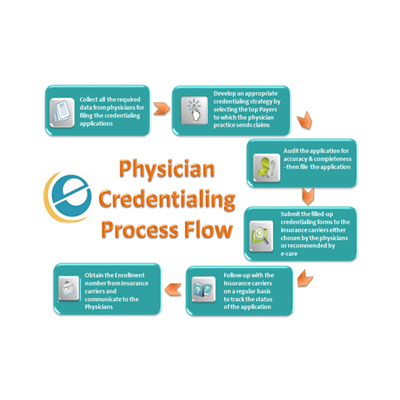
If you’ve ever watched a new provider sit on the sidelines for three months while their payer applications collect dust somewhere in a processing queue, you already know the frustration. Provider enrollment and credentialing is the kind of work that looks simple on paper but turns into a full-time job the moment you’re knee-deep in it.
At billcare, we’ve been doing this long enough to know where the process breaks down, which payers are slow, and what mistakes cause applications to come back rejected. This guide walks you through both processes honestly — what they involve, how long they realistically take, and how we manage them so you don’t have to.
Enrollment and Credentialing: They’re Related, But They’re Not the Same Thing
A lot of people use these terms interchangeably and that usually leads to confusion down the line. So let’s clear it up.
Credentialing is about verification. It’s the process of confirming that a provider is who they say they are and that they’re actually qualified to practice — education, training, board certifications, licensure, malpractice history, all of it. A hospital or insurance company won’t let a provider anywhere near their network without going through this first.
Enrollment is about authorization. Once a provider is credentialed, enrollment is what registers them with a specific payer so they can actually submit claims and get paid. You can be fully credentialed and still not enrolled — which means your claims go nowhere.
billcare manages both, and we run them concurrently wherever possible to cut down on the total timeline.
Why This Process Takes So Long (And Why That’s Not Always Your Fault)
Here’s something most people don’t realize: a significant chunk of the delay in enrollment and credentialing has nothing to do with you or your providers. Payers are slow. Credentialing committees meet once a month. PECOS applications sit in a CMS processing queue for weeks. CAQH profiles get flagged because of a minor data mismatch that nobody notices until an application comes back rejected.
What makes the difference is how proactively someone is following up, catching issues early, and keeping everything moving. That’s what billcare does.
The Enrollment Process, Step by Step
Here’s what a typical enrollment looks like when billcare manages it:
- We start with a complete intake — NPI, state license, DEA certificate, malpractice policy, CAQH credentials, and practice location details. We collect everything upfront so applications don’t stall halfway through.
- Our team prepares applications for each payer the provider needs to be enrolled with. Every payer has its own forms, its own portal, its own quirks. We know them.
- Applications go out. Then the tracking starts. We follow up with payer enrollment departments on a set schedule and escalate anything that’s been sitting too long.
- When approval comes through, we confirm the effective billing date, communicate it to your billing team, and update all relevant records.
- We also flag re-enrollment requirements well in advance so nothing lapses.
Commercial payers typically take 30 to 90 days. Medicare through PECOS can run 60 to 90 days, sometimes longer. We’re upfront about realistic timelines from day one.
The Credentialing Process, Step by Step
- Collect all provider credentials: degrees, residency documentation, board certifications, DEA registration, current state licenses.
- Build or update the provider’s CAQH ProView profile — this is what most payers pull from, so it needs to be complete and current.
- Run primary source verification directly with issuing institutions — we don’t take copies at face value.
- Submit credentialing applications to payers and hospital medical staff offices as needed.
- Track committee review timelines. If a committee meets monthly, we make sure the application is in before the cutoff.
- Once approved, we document the effective date and set re-credentialing reminders for 90 days before the deadline.
The Mistakes That Cause the Most Delays
After working through thousands of enrollments, the same problems come up again and again. Incomplete CAQH profiles. Outdated practice addresses in NPPES. Missing signatures on CMS-855 forms. Credentialing applications that get submitted without checking whether the provider has an active exclusion. These aren’t complicated problems — but they’re easy to miss when someone is managing 50 providers at once without a structured process.
billcare’s intake checklist and pre-submission review exist specifically to catch these issues before an application goes out, not after it comes back rejected.
How billcare Approaches This Work
We’re not a general billing company that does credentialing as a side service. Provider enrollment and credentialing is the core of what billcare does. Our team specializes in this work, which means faster turnaround, fewer errors, and direct payer contact that come from years of relationship-building.
Each client gets a dedicated account manager who knows your provider roster, tracks your applications, and is reachable when you have questions. No passing the buck to a general support line.
Frequently Asked Questions
Q: How far in advance should we start the enrollment and credentialing process?
A: At minimum, 90 days before a provider’s intended start date. For Medicare or Medicaid, give yourself 120 days. Starting early doesn’t speed up the payer — but it gives you a buffer when something comes back and needs to be corrected.
Q: Can billcare handle enrollment for an entire group practice at once?
A: Yes. We work with solo practitioners, mid-size group practices, and large health systems. The process scales — what changes is the volume of applications and the complexity of tracking, both of which we handle through our centralized management system.
Q: What happens if a payer rejects an application?
A: We analyze the rejection reason, correct the application, and resubmit. We communicate every rejection to you with a clear explanation of what happened and what we’re doing about it. You’re never left guessing.
Q: Do you handle re-credentialing when it comes up?
A: Absolutely. We track every re-credentialing deadline in our system and start the renewal process 90 to 120 days out. The goal is that you never get a termination letter because a re-credentialing deadline slipped through the cracks.
Q: Is enrollment the same as getting in-network with a payer?
A: Essentially, yes — but there’s nuance. Enrollment authorizes you to bill a payer. Whether you’re considered ‘in-network’ also depends on having an active, signed contract with that payer. billcare manages both the enrollment and the contracting side.